Center for Multiple Sclerosis Research
The Center for Multiple Sclerosis Research, housed within the Center for Neuropsychology and Neuroscience Research, focuses on investigating common impairments that affect individuals with MS, including mobility, cognition, fatigue, and well-being. Ongoing research examines the nature, trajectory, and approaches to manage these deficits, employing a variety of interventions that include neuroimaging, exercise, robotics, behavior modification, and pharmaceuticals.
Center Leadership
Center Leadership
-

Senior Vice President, Research and Training
Co-Director
Center for Multiple Sclerosis Research
Interim Director
-


News and Views from the Experts
Introducing milestones, the new multiple sclerosis (MS) research newsletter from Kessler Foundation. Here we’ll share information and insight on advances in the understanding and management of MS, including our current research.

Developing Strategies to Improve Memory
New learning, memory, and processing-speed deficits, common in MS, negatively impact everyday life. Two established cognitive rehabilitation protocols developed by Center scientists and supported by Class I research evidence, target specific cognitive functions and enhance the ability for individuals with MS to learn and remember. The two protocols are: Kessler Foundation Strategy-based Training to Enhance Memory (KF-STEM™) and Kessler Foundation modified Story Memory Technique (KF-mSMT®)
Join a Study Listen to RealTalkMS Interview: Nancy Chiaravalloti, PhD

Enhancing Cognition Through Exercise
Foundation researchers have accumulated strong evidence to support the use of physical exercise training—such as treadmill walking, cycling, and outdoor walking—to effectively restore functions that have been lost due to MS. Studies involve focusing on individual and synergistic effects of cognitive rehabilitation and exercise in individuals with relapsing-remitting and progressive MS.

Implementing Robotic Exoskeleton-Assisted Exercise
Robotic exoskeleton-assisted exercise rehabilitation represents a promising intervention approach for managing co-occurring mobility and cognitive impairments in individuals with substantial MS disability who might not benefit from traditional exercise rehabilitation. Our research aims to provide increased capacity to move or perform basic activities of daily living and improve quality of life.

Studying Quality of Life and Outcomes
Disease- and person-specific secondary factors from MS–such as depression, sleep disturbance, and personality changes–place significant demands on individuals’ ability to manage the illness and live fulfilling lives. Psychosocial interventions targeting MS symptoms and occupational outcomes are aimed at advancing self-efficacy, coping, and well-being through behavioral therapy and positive psychology techniques.
Join a Study: Reinventing Yourself Join a Study: Improving Psychological Well-Being

Exploring New Paradigms to Treat Cognitive Fatigue
Cognitive fatigue occurs after intense mental concentration such as a session of constant attention, learning, or problem-solving. Ongoing research focuses on understanding the neural mechanisms underlying fatigue to help diagnose and quantify cognitive fatigue in individuals with MS. Implementing rewarding activities, cognitive rehabilitation, mindfulness therapy, and disease-modifying medications are among the latest therapeutic strategies being tested.
Read More: Redefining MS Fatigue Treatments
Read ECTRIMS Interview: John DeLuca, PhD
Join an fMRI Study While Taking
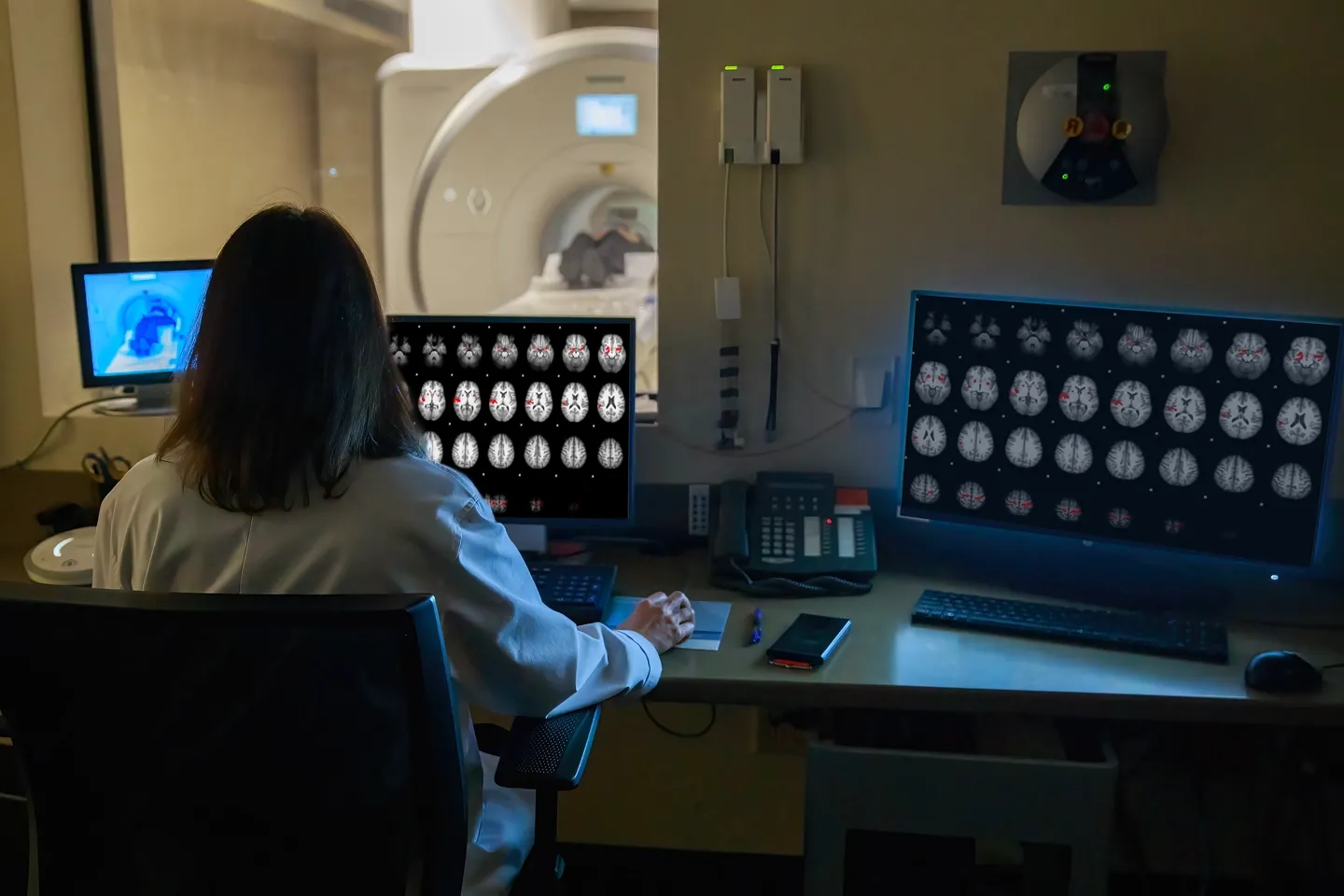
Visualizing Brain Activity with Functional Neuroimaging
Advanced multi-modality biomedical techniques allow Center researchers to visualize brain activity during specific tasks and sensations in individuals with MS, traumatic brain injury, and Parkinson's disease. Some of the techniques used include functional magnetic resonance imaging (fMRI), electroencephalography (EEG), and electromyography (EMG). The goal is to understand how cognitive rehabilitation can reshape memory-related brain regions and provide valuable insights into addressing cognitive and physical fatigue.

Relating Eye Movements and Processing-Speed Deficits
Although the visual symptoms associated with MS are well-documented, their impact has received limited attention. To address this issue, Center researchers are studying the link between eye movements and processing-speed deficits in MS and developing protocols for assessing cognitive function using eye trackers, irrespective of an individual’s motor abilities.