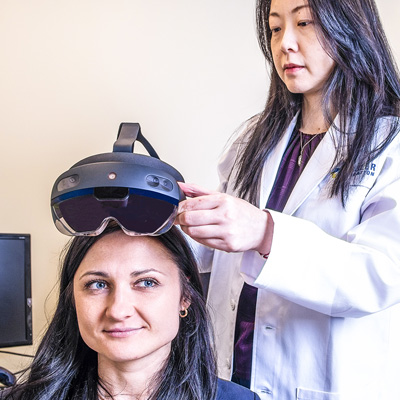
For Stroke Survivors
Stroke survivors with spatial neglect have a higher risk of falls, stay hospitalized longer, and have poorer rehabilitation outcomes than stroke survivors without spatial neglect.

For Family Caregivers
Assisting a family member who is a stroke survivor is a complicated task. The caregiver is a key member of the team. Arm yourself with as much information as possible. Know that you are not alone. The explanations, tips, and resources below will get you started.

For Professionals
Spatial neglect is a disorder resulting from a brain injury and frequently occurs after a stroke. According to Kessler Foundation’s research, more than 50% of stroke survivors admitted to rehabilitation hospitals are affected by spatial neglect and in need of effective treatment.
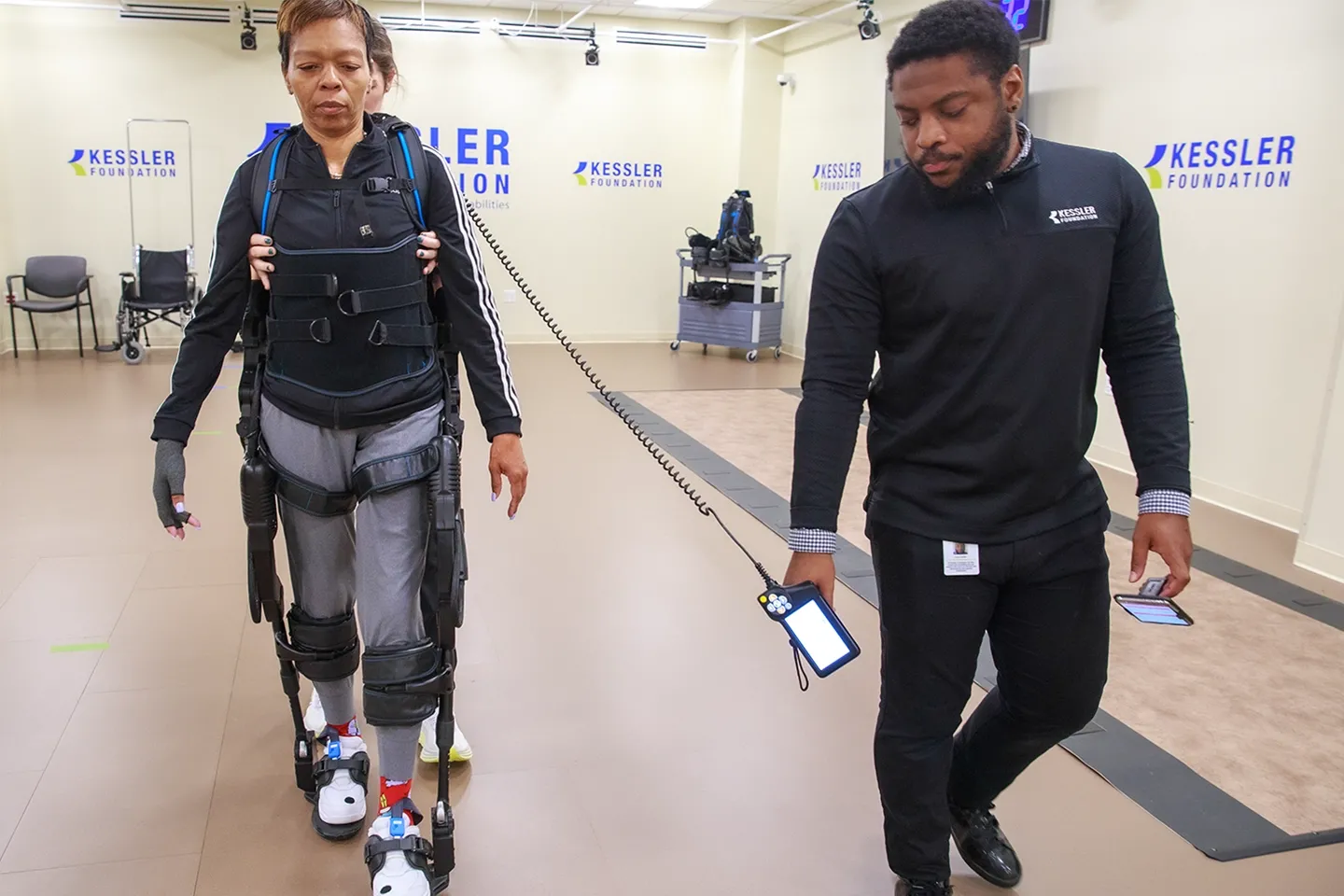
Volunteers are the Heart of Research